This web page was produced as an assignment for Genetics 564, an undergraduate course at UW-Madison

Human patients with major depressive disorder experience many sleep abnormalities including:
-persistent rapid eye movement (REM) delay
-increased REM density
-shorter total sleep time
-decreases in sleep efficiency [1]
A recent study in twin pairs discovered a correlation between sleep duration and depression. Those twins with a longer sleep duration had fewer depressive symptoms. The heritability of depressive symptoms among those who sleep eight hours a night was 27% while those who only slept five hours a night had a heritability of 53%. Those sleeping for ten hours a night had a heritability of depressive symptoms of 49%. This study indicates a relation between circadian rhythms and depression and warrants for future research [2].
-persistent rapid eye movement (REM) delay
-increased REM density
-shorter total sleep time
-decreases in sleep efficiency [1]
A recent study in twin pairs discovered a correlation between sleep duration and depression. Those twins with a longer sleep duration had fewer depressive symptoms. The heritability of depressive symptoms among those who sleep eight hours a night was 27% while those who only slept five hours a night had a heritability of 53%. Those sleeping for ten hours a night had a heritability of depressive symptoms of 49%. This study indicates a relation between circadian rhythms and depression and warrants for future research [2].
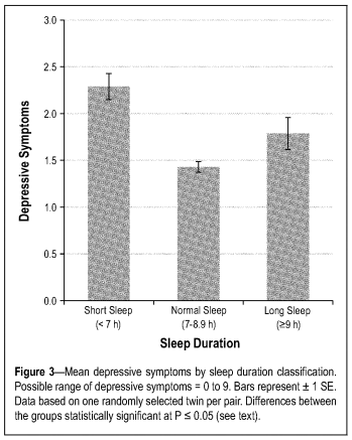
Twin studies are especially useful for determining if a variable (in this case, sleep duration) is genetically or environmentally determined. If reared together, twins share the same family background and typically also share childhood and adolescent exposures [3]. This study indicated that sleep durations outside the normal range increased the genetic risk for depressive symptoms (see figure at left from [3]). Therefore, normalization of sleeping habits may reduce genetic risk for depression and serve as a therapy for those experiencing depressive symptoms. It is important to note that the majority of the twins in this study were younger adult Caucasian women and therefore we must use caution in applying these results to the general population [3].
References
[1] Li, J., et al. (2013). Circadian patterns of gene expression in the human brain and disruption in major depressive disorder. PNAS. 110(24). doi:10.1073/pnas.1305814110
[2] Piper, L. (2014, February 17). Sleep duration impacts on genetic risks of depressive symptoms. medwire News. Retrieved from http://www.medwirenews.com/55/105355/Affective_disorders/Sleep_duration_impacts_on_genetic_risk_of_depressive_symptoms.html
[3] Watson, N., et al. (2014). Sleep Duration and Depressive Symptoms: A Gene-Environment Interaction. SLEEP. 37(2). doi:10.5665/sleep.3412
[1] Li, J., et al. (2013). Circadian patterns of gene expression in the human brain and disruption in major depressive disorder. PNAS. 110(24). doi:10.1073/pnas.1305814110
[2] Piper, L. (2014, February 17). Sleep duration impacts on genetic risks of depressive symptoms. medwire News. Retrieved from http://www.medwirenews.com/55/105355/Affective_disorders/Sleep_duration_impacts_on_genetic_risk_of_depressive_symptoms.html
[3] Watson, N., et al. (2014). Sleep Duration and Depressive Symptoms: A Gene-Environment Interaction. SLEEP. 37(2). doi:10.5665/sleep.3412
